When the Rules Don’t Fit, He Rewrites Them
UVM Medical Center surgeon challenges long-held norms to help more patients move without pain.

For years, orthopedic surgeons followed guidance recommending that joint replacement be delayed for patients with a body mass index (BMI) over 40 because of a slightly increased risk of complications. Like many of his colleagues, University of Vermont Health – UVM Medical Center orthopedic surgeon Michael Blankstein, MD, used those guidelines when counseling patients. But over time, he began to question whether they were truly serving the people in front of him — or simply shutting them out.
Today, his academic work is prompting a shift in how orthopedists nationwide think about surgical eligibility for patients with obesity, helping more people reclaim their lives from chronic joint pain. In a field where long-standing norms often go unchallenged, his findings are already influencing conversations about what equitable, compassionate care should look like.
Brittany Granara, NP, who works closely with Dr. Blankstein in the arthroplasty program, says the shift reflects his dedication. “He’s always looking to improve his practice and his patients’ outcomes,” she says. “He cares deeply about the work. It’s all about what serves patients best.”
A Collaborative Approach
Dr. Blankstein brings energy and clarity to patient conversations. When discussing something serious, like an upcoming knee replacement, his direct style builds trust. He’ll tell you plainly: he feels lucky to do this work. Helping people move without pain is what drew him to medicine as a child, when he first watched his father put a cast on a classmate’s broken arm.
Since then, he’s built a career spanning clinical care, medical education, research and national advocacy.
“He’s passionate about his role as a surgeon, but also as an educator and researcher,” says Granara. “He’s constantly thinking about how to improve outcomes beyond the OR.”
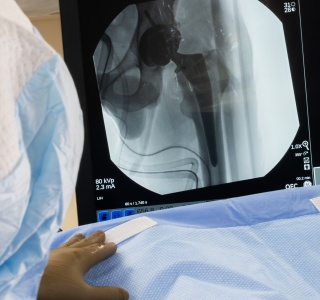
At UVM Medical Center, where he’s one of the leaders in the Hip and Knee Surgery Program, Dr. Blankstein focuses on joint replacement surgery — procedures that can transform lives. Patients who have spent years in pain walk again, returning to activities they love and often experiencing a lift in mental health.
But many of those patients were once turned away because of their weight.
“Doc, you gotta be kidding me. You’re telling me I need to lose 50 pounds when I can’t even walk five steps?” one patient told him. Others left in tears. “Those conversations,” Dr. Blankstein says, “were some of the saddest I’ve ever had.”
Rethinking the Rules
Those moments pushed him to reexamine the evidence behind strict BMI cutoffs. What he found surprised him. While patients with a BMI over 40 do have a modestly higher risk of infection, the increase is relatively small, and nowhere near the absolute barrier the guidelines implied. Meanwhile, patients with other meaningful risk factors — such as diabetes, kidney dysfunction, autoimmune and heart disease — continued to move forward with surgery.
To Dr. Blankstein, it didn’t make sense to apply one rigid threshold to just one group.
He also realized how those blunt restrictions landed with patients. “This is already a population that hears the word ‘no’ a lot,” he says. “The last thing we want to do in health care is add to that chorus."
That is when he changed course.
When Lori Richardson, 55, of Tupper Lake, met Dr. Blankstein for the first time, she braced for another rejection. Instead, she remembers his encouragement. “He said, ‘We will do this. I’ll do my part, but I’m going to need you to do your part.’ After being told no because of my weight, hearing that felt like a light at the end of the tunnel.”
Richardson's experience reflects Dr. Blankstein’s new approach. Rather than setting a strict cutoff, he begins with a respectful question: Is it okay if we talk about your weight? If patients are willing, his team works with them to reduce modifiable risk factors — quitting smoking, improving blood sugar control, or trying new weight-loss medications. But there’s no mandated weight goal.
"Numbers can be daunting,” he says.
He asks patients to return in three months, but the focus is on shared decision-making, not a target. “The most important goal,” he says, “is for us to have a relationship.”
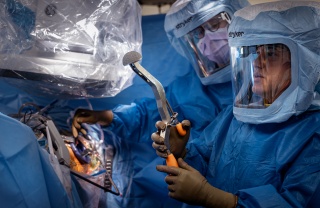
Seeing the Whole Person
The team-based approach is now standard in the UVM Health Hip and Knee Surgery Program. Health coaches, nurses, endocrinologists and surgeons collaborate to prepare patients for surgery in ways that support long-term health. It’s a shift toward more personal and sustainable care.
At the same time, he’s thinking about broader trends. By 2030, more than half of U.S. adults are expected to be obese, with the highest burdens on people already facing systemic barriers: low-income patients, women and communities of color.
“You have people in chronic, debilitating pain,” he says. “They’re depressed, they can’t move – and you tell them, ‘come back when you’ve lost 50 pounds.’”
In his experience, many don’t lose the weight. But they do lose hope.
“Being obese is not a personal choice,” he says. “It’s a societal problem. I want to be part of changing how we talk about eating and health in this country.”
His research on rethinking BMI cutoffs has received national attention, and he continues to share emerging evidence through publications, lectures and his podcast. At University of Vermont's Larner College of Medicine, where he recently received the Teacher of the Year Award, he brings those lessons to future physicians.
For Dr. Blankstein, the work always comes back to partnership.
I tell patients, ‘I’m your friend for life,’” he says. “I mean that. It has to be a partnership. That’s what inspires me.
His patients feel it. A year after her second hip replacement, Richardson says she is stronger than she has been in a decade. “I was in a wheelchair. I couldn’t walk up stairs. I had to go live with my dad,” she says. “Now I’m strutting around like a rock star!”
At a recent follow-up, she says Dr. Blankstein walked in with a proud smile at her incredible progress. “I wasn’t sure whose grin was bigger,” says Richardson, “mine or his!”

