
The Beat
Taking the pulse on patient care, innovation and wellness.



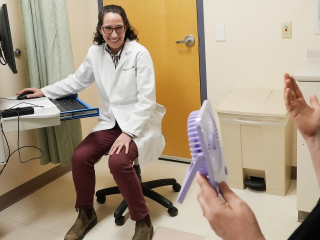
Exceptional Care
Where medical excellence and human kindness meet.


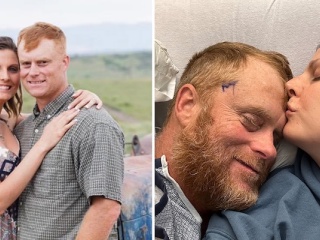
Innovation & Impact
Tackling tough challenges with advanced research and education, new technology and visionary thinking.
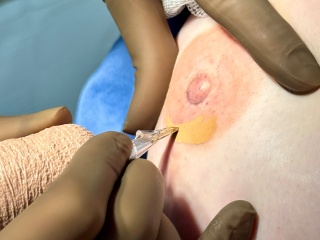

Our People
Celebrating the individuals who bring our mission to life.




Health & Wellness
Trusted, practical advice to inspire a healthy lifestyle.
For years, Continuous Glucose Monitors were used almost exclusively in diabetes care. As technology has improved, interest has expanded well beyond that original purpose.
When the temperatures drop, viruses get busy. Here's your quick guide to flu, COVID and RSV.
Join us as we dive into the concept of Culinary Medicine, a paradigm-shifting approach to food and wellness.
Aerobic activity may protect your brain — it’s even more important as we age.
Media Center
The latest news and facts about University of Vermont Health.


