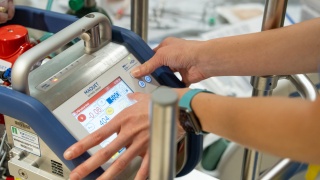
Precision Under Pressure
Preparing for when a patient’s heart and lungs fail.

Some moments in medicine are so precarious that a life can tip in either direction. Few are as delicate as when a person’s heart and lungs can no longer sustain them. In those rare and critical moments, a highly trained team turns to one of modern critical care’s most complex tools: ECMO.
“ECMO offers a crucial bridge between medical crisis and the possibility of recovery,” says Erica Charkalis, a nurse practitioner in the cardiovascular intensive care unit of University of Vermont Health - UVM Medical Center. “It can give someone a chance to heal just enough so that they can move to a longer-term course of treatment and recovery. It can be a game changer for our most seriously ill patients.”
Charkalis is part of a multidisciplinary team of ECMO specialists, including nurses, advanced practice providers, physicians, surgeons, respiratory therapists and perfusionists. Their readiness depends on regular simulations to help them prepare for the urgent moments of true ECMO emergencies.
Low-Pressure Training for High Stakes Moments
“We’ve got a flow alarm going off, her blood oxygen is crashing — what do we do?” asks Terry Setien, a critical cares nurse clinician and coordinator of the ECMO program. After four decades in critical care, Setien guides these scenarios with steady calm. “Take your time, this is why we train — so we’re ready if and when this happens in real life.”
Around her, a small group of ICU physicians and nurses huddle over a blue-haired mannequin connected to the compact machine capable of taking over a person’s heart and lung functions. At her side is Paul Hunter, UVM Medical Center’s chief perfusionist and, as Setien calls him, her “partner in crime” for the hospital’s bimonthly ECMO drills.
“To offer this service 24/7, we need a team capable of troubleshooting the complex issues that can occur when a person is on ECMO,” Hunter says. “These low-pressure trainings keep us sharp and expand the pool of clinicians who can safely help our patients.”
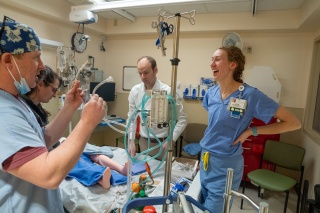
Perfusionists manage heart–lung support systems during cardiac surgery and run advanced life-support therapies like ECMO. Because the hospital only has a small number of them, a growing number of ICU nurses have stepped forward to hone their skills and provide this life-saving support, especially overnight or during weekends. Thirty-two nurses and two respiratory therapists are now in training.
Among them is Alicia Imbergamo, RN, who attended the session after caring for an ECMO patient last summer.
“This level of care is hardly routine, so these simulations build confidence,” she says, as she studies the network of tubes and wires keeping their mannequin “alive.” When another alarm sounds, Imbergamo pivots to the ECMO machine, working through the problem under Hunter's guidance.
A Lifeline, Close to Home
Though ECMO is used only in the most severe cases, its availability in Vermont provides a critical lifeline to a higher level of care that would otherwise require traveling hundreds of miles for care.
Without this program, our patients would need to go to Boston or New York. That can be a real burden, and for many, it’s simply not an option. They may not survive the trip.
Professionally, the program offers clinicians a chance to practice at the pinnacle of intensive care medicine without leaving the state.
“These cases are so complex and require so much collaboration,” Charkalis says. “I dreamed of working at this level, at the top of my license. It’s fantastic to do that right here at home in Vermont.”