Health Library
Asthma in children – Discharge instructions
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
What are discharge instructions?
Discharge instructions are information about how to take care of your child after getting medical care for a health problem.
What is asthma?
This is a condition that can make it hard to breathe. The symptoms can be mild or severe. They can come and go. An asthma "attack" is when symptoms start suddenly. This happens when the airways in the lungs become more narrow and inflamed (figure 1)
Asthma can run in families.
How do I care for my child at home?
Ask the doctor or nurse what you should do when you go home. Make sure you understand exactly how to care for your child. Ask questions if there is anything you do not understand.
You should also:
● Give your child all their medicines as instructed – Their doctor might prescribe:
● Quick-relief medicines – These open the airway quickly to stop symptoms of an asthma attack in 5 to 15 minutes. Everyone with asthma should have a quick-relief inhaler to use during an asthma attack. Carry it with you at all times. Make sure all caregivers always have 1 with them.
Most people rarely need their quick-relief medicines. But some might need them 1 or 2 times a week. When asthma symptoms get worse, more doses might be needed. Some children get hyperactive and have trouble staying still after taking these medicines. But this usually does not last very long.
● Long-term controller medicines – These reduce inflammation in the long term to help prevent asthma symptoms from happening. If your child needs controller medicines, they should take them every day, even if they have no symptoms. Their doctor might tell you to give your child controller medicine if, for example, your child has asthma symptoms that bother them often or that are more severe. When these medicines are working well, your child's asthma symptoms are controlled, and they should not need quick-relief medicines very often.
● Steroids that come as pills or liquid – If your child's asthma symptoms are more severe, they might need to take steroid pills for a few days or weeks.
Many children have 1 inhaler for quick relief medicine and 1 for long-term controller medicine. Some have 1 inhaler for both. Almost all children with asthma use an inhaler with a device called a "spacer." Younger children might need a machine called a "nebulizer" to breathe in their medicine. The spacer and nebulizer both help get more medicine into the lungs (figure 2). The doctor or nurse will show you how to use them.
● Avoid "triggers" – These are things that make your child's symptoms worse. Common triggers include tobacco smoke, smoke from wildfires, air pollution, allergens (such as dust, mold, pollen, or pet hair), strong chemicals or smells, and very cold or dry air. Exercise and stress can also be triggers. But do not have your child stop exercising, unless they are sick or getting over a flare. This is because exercise is important for staying healthy. Also, regular exercise and better fitness can actually help reduce asthma symptoms.
If your child cannot avoid certain triggers, talk with their doctor about what they can do. For example, they might need to take an extra dose of their quick-relief inhaler medicine before exercising or being around things they are allergic to.
● Avoid smoking around your child – Do not let others smoke near your child. Smoke can stay on clothes and furniture, and cause breathing problems. If you are having trouble quitting smoking, your doctor or nurse can help.
● Lower your child's risk of getting sick – In children, viral infections are the most common asthma trigger. Examples include colds, the flu, and COVID-19.
It's important children get the COVID-19 and flu vaccines. This lowers the risk of severe illness if they get one of these infections.
● Follow your child's "asthma action plan" (form 1) – This is a list of instructions that tell you:
● What medicines your child should use at home each day
● What symptoms to watch for that could mean their asthma is getting worse
● What other medicines to give your child if their symptoms get worse
● When to get help or call for an ambulance
Ask your child's doctor to help you make an asthma action plan if you don't have one.
What follow-up care does my child need?
The doctor or nurse will tell you when your child should follow up with their regular doctor. This is usually within 1 week.
If your child needs asthma medicine every day, they should see their doctor or nurse regularly. For many children, this means every 3 to 6 months. At these appointments, the doctor or nurse will ask about your child's symptoms, check how well their lungs are working, and talk about their treatment plan.
When should I call the doctor?
Call for emergency help right away (in the US and Canada, call 9-1-1) if your child has severe symptoms, like:
● They have so much trouble breathing they cannot talk.
● The skin and muscles around their ribs are pulling in with each breath (called "retractions").
● Their lips or fingernails turn gray or blue.
● They are very drowsy or not responding normally.
Call for advice if:
● Your child uses a quick-relief medicine for an asthma attack, and their symptoms do not improve, get worse, or come back quickly.
● Your child needs to use their quick-relief medicine more than 2 times a week.
● Your child cannot do their normal activities because of their asthma symptoms.
● You have any questions about your child's medicines.
Teach back
The "teach-back method" is a way to make sure you understand the information you received. This means being able to explain what you learned in your own words.
After reading the information above, think about how you would answer these questions:
● What is my child's condition or health problem?
● How do I care for my child, and why is this important?
● What problems should I watch for, and when should I call the doctor?
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Apr 04, 2026.
Topic 145451 Version 4.0
Release: 34.3.4 - C34.92
Images
figure 1: Asthma
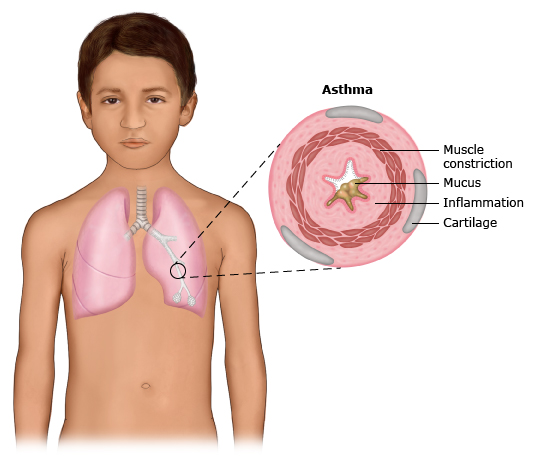
During an asthma attack or flare-up, the muscles around the airways tighten (constrict), and the lining of the airways gets inflamed. Then, mucus builds up. All of this makes it hard to breathe.
Graphic 65956 Version 11.0
figure 2: Using a valved holding chamber or other spacer device
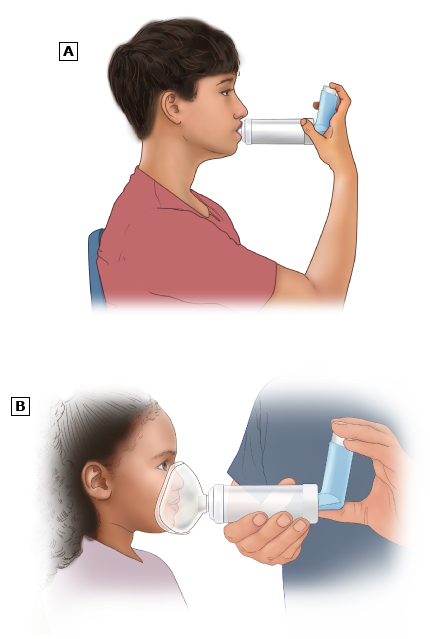
Most children with asthma use an inhaler with a valved holding chamber or other spacer device. This is a device that attaches to the inhaler's mouthpiece. The devices shown in this figure are both valved holding chambers.
(A) When the child presses down on the canister, a puff of medicine is released into the valved holding chamber/spacer. Then, the child breathes it in.
(B) Some valved holding chambers/spacers come with a face mask. If your child's valved holding chamber/spacer has a mask, hold it snugly over their mouth and nose. Then, press down on the canister to release the medicine into the valved holding chamber/spacer. The child can then breathe it in.
Graphic 75577 Version 12.0
form 1: Asthma action plan (child)
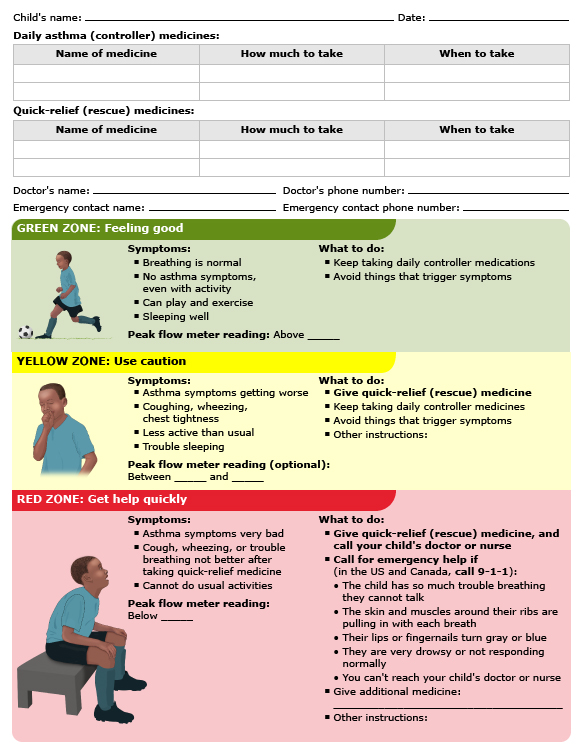
An asthma action plan is a list of instructions that tell you:
What medicines to give your child at home each day, if any
What symptoms to watch for
What other medicines to give your child if their symptoms get worse
When to call the doctor or get emergency help
Graphic 140837 Version 3.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.