Health Library
Kidney disease caused by diabetes
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
Can diabetes cause kidney disease?
Yes. People with diabetes have an increased risk of kidney disease. This is called "diabetic kidney disease."
The kidneys filter blood and remove waste and excess salt and water (figure 1). In people with kidney disease, the kidneys slowly lose the ability to filter blood. With time, the kidneys can stop working completely.
What are the symptoms of kidney disease caused by diabetes?
At first, kidney disease causes no symptoms. But as the disease gets worse, it can:
● Make your feet, ankles, or legs swell (called "edema")
● Cause high blood pressure
● Make you very tired
● Damage your bones
Is there a test for kidney disease?
Yes. Your doctor can do urine and blood tests to check how well your kidneys are working.
If you have diabetes, your doctor will check your kidneys regularly. If you do have kidney disease, regular tests can show if it is getting worse over time.
What can I do on my own to protect my kidneys?
If you have diabetes, there are things you can do to lower your risk of kidney disease. If you already have kidney disease, these things can also help slow it down.
You should:
● Manage your blood sugar – This includes taking your diabetes medicines as instructed. It also includes lifestyle changes, such as:
● Eating a healthy diet
● Getting regular physical activity
● Quitting smoking, if you smoke
● Losing weight, if you have excess body weight
● Avoiding or limiting alcohol
● Keep your blood pressure as close to normal as possible – People with diabetes and kidney disease often have high blood pressure, too. This can make kidney disease worse. It also increases your risk of heart disease and stroke. Your doctor or nurse will talk to you about how to manage your blood pressure. This includes lifestyle changes and usually medicines.
● Limit medicines that can harm the kidneys – One example is nonsteroidal antiinflammatory drugs ("NSAIDs"). These include ibuprofen (sample brand names: Advil, Motrin) and naproxen (sample brand name: Aleve). There are other medicines that people with kidney disease need to avoid, too. Check with your doctor before starting any new medicine or supplement, even ones you can buy without a prescription.
● Go to all your medical appointments – If you have diabetes and kidney disease, your doctor will probably want to see you every few months. If your kidney disease gets worse over time, you will probably need to see a kidney specialist, called a "nephrologist."
What other treatment might I have?
Depending on how severe your kidney disease is, your doctor might prescribe medicines. Medicines cannot reverse kidney disease, but they can help slow it down.
Examples include:
● An "ACE inhibitor" or "angiotensin receptor blocker"
● An "SGLT2 inhibitor" – You might get this type of medicine if you have type 2 diabetes and kidney disease. Examples include canagliflozin (brand name: Invokana), empagliflozin (brand name: Jardiance), and dapagliflozin (brand name: Farxiga).
● A "GLP-1 receptor agonist"– You might get this type of medicine if you have type 2 diabetes and kidney disease. GLP-1 medicines include semaglutide (brand names: Ozempic, Wegovy) and tirzepatide (brand name: Mounjaro, Zepbound).
● Finerenone (brand name: Kerendia) – You might get this medicine if you have type 2 diabetes and kidney disease.
● Medicines to help lower blood sugar
Your doctor might prescribe other medicines, too. Your treatment plan might change over time if your kidney disease gets worse.
What if I want to get pregnant?
Talk to your doctor before you start trying. Kidney disease can increase the risk of problems during pregnancy. Also, some of the medicines used for kidney disease are not safe during pregnancy.
Your doctor can work with you to manage your kidney disease and plan for pregnancy.
What happens if my kidneys stop working completely?
In people with kidney disease, their kidneys slowly lose the ability to filter blood. When they mostly or completely stop working, it is called "kidney failure" or "end-stage kidney disease." This can happen after many years, or sooner.
Some people can prevent end-stage kidney disease with medicines and lifestyle changes.
If your kidneys can no longer filter blood properly, your treatment choices are:
● Kidney transplant – This is surgery to put a healthy kidney into your body. The new, healthy kidney then does the job of the diseased kidneys. (People need only 1 kidney to live.)
● Dialysis – This is a treatment that takes over the job of the kidneys. Some people get dialysis while they wait for a kidney transplant. Otherwise, dialysis can be continued for the rest of your life. There are 2 types of dialysis:
● Peritoneal dialysis – This is a procedure you do at home every day. It involves piping a special fluid into your belly. This fluid collects waste and excess salt and water from your blood. Then, the used fluid drains out of your belly.
● Hemodialysis – This is a procedure in which a dialysis machine takes over the job of the kidneys. The machine pumps blood out of your body, filters it, and returns it to your body. You need to have hemodialysis at least 3 times a week.
Some people choose not to have a kidney transplant or dialysis. Without either of these treatments, end-stage kidney disease eventually leads to death. This usually happens quickly, within days to weeks. But it can take longer. If you choose not to have a kidney transplant or dialysis, you can still get care to help make you more comfortable.
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Mar 20, 2026.
Topic 143770 Version 4.0
Release: 34.2.3 - C34.77
Images
figure 1: Anatomy of the urinary tract in adults
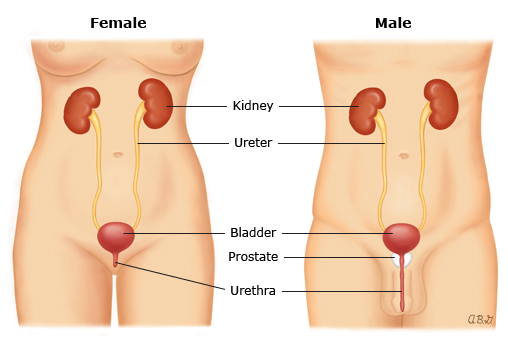
Urine is made by the kidneys. It passes from the kidneys into the bladder through 2 tubes called the "ureters." Then, it leaves the bladder through another tube called the "urethra."
Graphic 79864 Version 10.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.