Health Library
Foot care for people with diabetes
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
Why is foot care important if I have diabetes?
Diabetes can cause nerve damage if your blood sugar is high for a long time. This is called "diabetic neuropathy."
If you have problems with the nerves in your feet, you might not be able to feel pain in your foot. Normally, people feel pain when they get a cut or a blister on their foot. The pain tells them they need to treat their cut so it can heal. But people with nerve damage might not feel any pain when their feet get hurt. They might not even know they have a cut, so they might not treat it. Problems that aren't treated right away can get much worse. For example, an untreated cut can get infected and turn into an open sore.
High blood sugar can also damage blood vessels and decrease blood flow to your feet. This can weaken your skin and make wounds take longer to heal. You are also more likely to get an infection if you have high blood sugar.
How do I take care of my feet?
Taking good care of your feet can help prevent foot problems. You should:
● Wash your feet every day with soap and warm water. Pat your feet dry, and dry the skin between your toes.
● Keep your feet moisturized. Put lotion on the tops and bottoms of your feet, but not between your toes.
● Check your feet every day (figure 1). Look for cuts, blisters, redness, or swelling. Use a mirror, or ask someone to help you check the bottoms of your feet. Check all parts of each foot, especially between the toes. Look for broken skin, ulcers, blisters, or redness.
● Trim your toenails straight across when needed (figure 2). Do not cut the corners of your toenails. File rough edges. Do not cut your cuticles. Ask for help if you cannot see well or have problems reaching your feet.
● Ask your doctor or nurse to check your feet at each visit. Take your shoes and socks off for these checks.
● See a foot care provider (such as a podiatrist) if you have an ingrown toenail, corn, or callus. Do not try to remove corns and calluses yourself.
How do I protect my feet from injury?
There are several ways to protect your feet. You should:
● Wear shoes and socks at all times, even at home. Do not walk barefoot. Wear swim shoes if you go to the beach or a swimming pool.
● Choose shoes that fit well. They should not be not too tight or too loose. Your shoes should have plenty of room for your toes (figure 3). Your doctor might give you a prescription for special shoes. Check to see if they are covered by your insurance.
● Check your shoes each time before you put them on to make sure the lining is smooth. Also check to make sure there is nothing inside the shoes before putting them on.
● Avoid shoes that expose any part of your foot, like sandals, thongs, or clogs.
● Wear wool or cotton socks that fit loosely. Do not wear shoes without socks.
● Protect your feet from heat and cold. Test bath water before putting your feet in to make sure it is not too hot. Do not walk barefoot on hot ground. Take extra care when going outside in the cold, and wear warm socks.
What else should I know?
You can lower your risk of foot problems by keeping your blood sugar levels as close to your goal as possible.
Other things you can do include:
● Move your ankles and toes often to help with blood flow. You can wear a support stocking to help with swelling.
● Walk often. This helps blood flow. It is also good for your overall health.
● Quit smoking, if you smoke. Your doctor or nurse can help. Smoking causes poor blood flow to the feet and can damage nerves.
When should I call the doctor?
Call your doctor or nurse for advice if you have:
● A fever of 100.4°F (38°C) or higher, chills, or a wound that will not heal
● Swelling, redness, warmth around a wound, a bad smell coming from a wound, or yellowish, greenish, or bloody discharge
● Sores or blisters on your feet that hurt more or less than you would expect
● Numbness or tingling in your foot or leg
● Corns, calluses, blisters, or new sores on your foot
● Very dry, scaly, or cracked skin on your feet
● Changes in how your foot joints or arch look
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Apr 28, 2026.
Topic 142206 Version 5.0
Release: 34.3.4 - C34.116
Images
figure 1: Foot check for people with diabetes
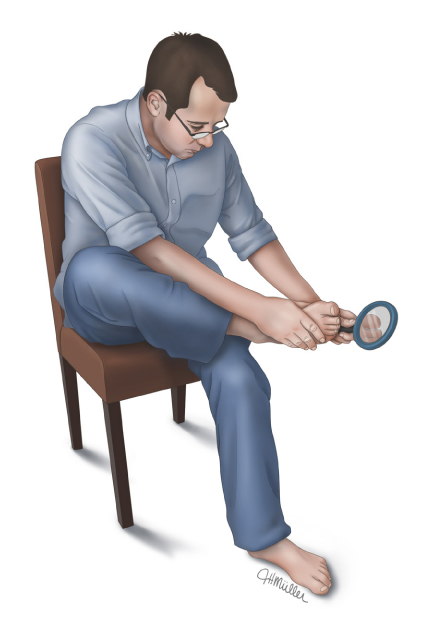
People with diabetes should check both of their feet every day.
It is important to check your feet all over, including in between your toes. If you can't see the bottom of your foot, use a mirror or ask another person to check for you. Tell your doctor or nurse if you see any:
Redness
Cuts or cracks in the skin
Blisters
Swelling
Graphic 77032 Version 5.0
figure 2: Trimming toenails
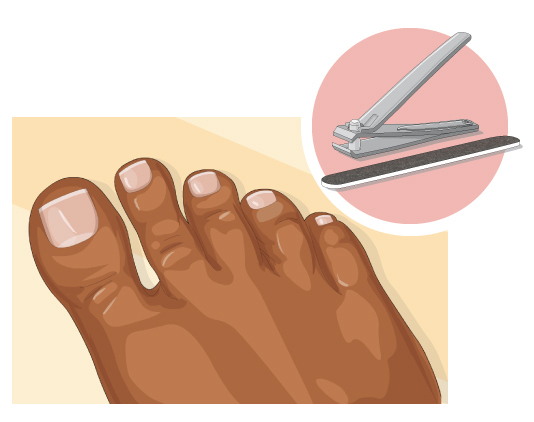
Trim your toenails straight across, and smooth them with a nail file.
Graphic 80053 Version 3.0
figure 3: Correct shoe shape
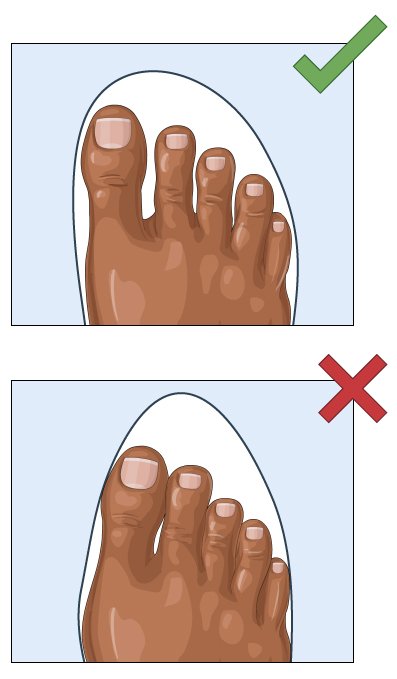
Choose shoes that fit well and are not too tight or too loose. Your shoes should have plenty of room for your toes.
Graphic 79305 Version 3.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.