Health Library
Obstructive sleep apnea in children
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
What is obstructive sleep apnea?
Obstructive sleep apnea, or "OSA," is a condition that makes a person stop breathing for short periods while they sleep. The person stops breathing because their throat narrows or closes.
Both children and adults can have OSA. In children, it often happens when the tonsils or adenoids are larger than normal (figure 1). These are areas of soft tissue in the back of the throat. If they are large, they can block the airway during sleep. Other conditions, including having excess body weight and certain medical problems, also increase a child's risk of OSA.
There are other types of sleep apnea, too. But OSA is the most common.
What are the symptoms of OSA?
OSA causes symptoms both at night and during the day.
At night, your child might:
● Snore
● Breathe loudly or have trouble breathing
● Have pauses between breaths or suddenly gasp for breath
● Breathe through their mouth
● Seem restless or move around a lot
● Sweat a lot
● Wet the bed or wake up often to urinate
● Sleepwalk or have "night terrors"
During the day, your child might:
● Wake up with a headache
● Feel very tired
● Fall asleep at unusual times, like at school or on a short car ride
● Breathe through their mouth
● Have trouble focusing in school
● Act grumpy or irritated
Should my child see a doctor or nurse?
Yes. If you think your child might have OSA, talk to their doctor. The doctor will do an exam and ask about your child's symptoms and sleep habits. They will probably also look into your child's mouth and throat.
The doctor might also suggest taking your child to see another doctor. This could be an expert in sleep problems or "ear, nose, and throat" medicine.
Is there a test for OSA?
Yes. If a doctor suspects your child has OSA, they might suggest a "sleep study." For this, your child spends the night in a room called a "sleep lab." In the lab, your child sleeps in a bed while they are hooked up to different machines. The machines record your child's heart rate, breathing, and other body functions.
In some cases, doctors can tell a child has OSA without doing a sleep study.
How is OSA in children treated?
There are 2 main treatments:
● Surgery to remove the tonsils or adenoids – If your child's tonsils or adenoids are larger than usual, OSA is often treated with surgery to remove them. This surgery is called "adenotonsillectomy."
If OSA is not severe, another option is to wait a few months before deciding about surgery. Your child's symptoms might improve with time and other changes. For example, getting treatment for allergies or asthma sometimes helps. For children with excess body weight, changing their diet and exercise habits might improve OSA symptoms.
● Positive airway pressure ("PAP") – This is a device that keeps your airway open while you sleep. People getting PAP wear a face mask at night that keeps them breathing. There are different types of PAP devices, including "CPAP" and "BPAP."
PAP might be suggested if your child's tonsils and adenoids are normal size, if surgery is not an option, or if surgery did not help with symptoms. Other times, doctors suggest a few weeks of PAP treatment before adenotonsillectomy.
For PAP treatment, your child wears a mask over their nose during sleep. The mask connects to a machine that keeps air flowing and helps keep your child's airway open (figure 2).
If your child's doctor recommends a PAP machine, be patient about helping your child learn how to use it. It can take time for a child to get used to wearing the mask and sleeping with the machine. Talk to your child's doctor or nurse if you are having trouble. They can give you tips on how to make the process easier, and can check the mask to make sure it fits right, or try a different type of mask.
Some children need other treatments, too. For example:
● Children with a narrow palate (roof of the mouth) might need to see an orthodontist. It sometimes helps to get a device that can widen the palate and make it easier to breathe during sleep.
● For children with seasonal allergies, doctors might suggest medicines to help with a stuffy nose.
What can I do on my own to help my child?
In addition to the above treatments, there are some other things that might help. You can:
● Keep your home free of smoke – Do not smoke in your home or let others smoke. Smoke can make OSA symptoms worse.
● Get treatment for asthma or allergies – If your child has asthma or seasonal allergies, make sure they use any treatments their doctor prescribed. Also, talk to their doctor or nurse about how to avoid "triggers." These are things that make the asthma or allergy symptoms worse. Triggers might include dust, mold, pets, pollen, or viral illnesses like a cold or the flu.
● Help your child lose weight, if they are overweight – Being overweight or having obesity makes OSA worse, so losing weight can help improve symptoms. Your child's doctor or nurse can give you tips on how to help your child lose weight safely. If your child is not overweight, losing weight will not help, and could even be harmful.
● Help your child avoid sleeping flat on their back – For older children who seem to have more symptoms when they sleep flat, changing position can sometimes help with breathing at night. You can try using blocks to raise the head of your child's bed. There are also special pillows and devices designed to help keep a person in 1 position. Talk to your child's doctor or nurse if you want to try this.
Can OSA lead to other problems?
Yes. If it is not treated, OSA can make a child very tired during the day. Over time, this can affect:
● Learning – This can include trouble thinking clearly, focusing, and performing in school.
● Mood and emotions – Children might act grumpy, irritable, or angry. They might also have depression or anxiety.
● Behavior – Some children have trouble controlling their behavior. They might act restless and have trouble sitting still.
● Growth – In severe cases, children with OSA might not grow as quickly as they should.
● Heart function – Over time, OSA can lead to heart problems. These can include a heartbeat that is faster than normal or high blood pressure.
Getting treatment for your child's OSA can help them feel better and prevent these problems.
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Apr 08, 2026.
Topic 120355 Version 10.0
Release: 34.3.4 - C34.96
Images
figure 1: Tonsils and adenoids
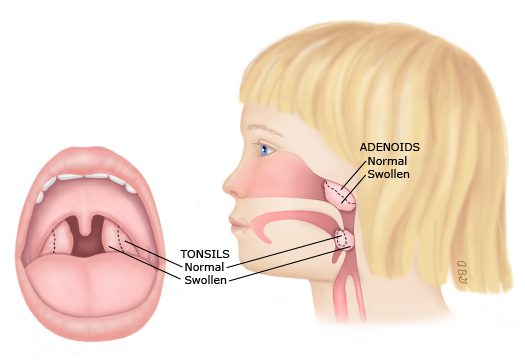
The tonsils and adenoids are areas of soft tissue in the back of the throat. If they get swollen, they can keep a child from breathing normally through the mouth or nose.
Graphic 119936 Version 1.0
figure 2: Positive airway pressure ("PAP") for obstructive sleep apnea
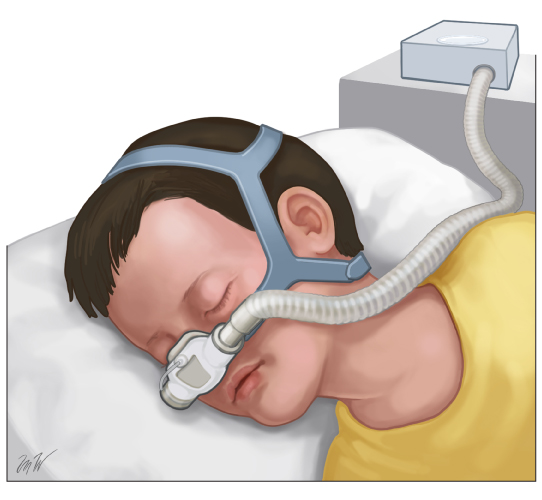
The PAP mask gently blows air into the child's nose while they sleep. It puts just enough pressure on their airway to keep it from closing.
Graphic 120554 Version 3.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.