Health Library
Exercise-induced asthma
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
What is exercise-induced asthma?
This is when a person with asthma has breathing problems during or after exercise. It is also called "exercise-induced bronchoconstriction." That's because exercise does not actually cause asthma. But it can trigger symptoms in some people who already have asthma.
Some people have no other symptoms of asthma. They only need treatment for the breathing problems that happen with exercise.
What are the symptoms of exercise-induced asthma?
Symptoms can include:
● Coughing
● A tight feeling in the chest
● Shortness of breath
● Wheezing (a whistling sound when breathing)
In people with exercise-induced asthma, exercise causes the airways in the lungs to narrow (or "constrict") (figure 1). This causes asthma symptoms about 10 to 15 minutes after starting to exercise. In most cases, the symptoms go away after about 1 hour.
These symptoms are different from shortness of breath that happens during an asthma "attack." This is when symptoms start suddenly. A person having an asthma attack might have more trouble breathing if they try to exercise. That's because their airways are already narrowed.
Is there a test for exercise-induced asthma?
Yes. But if you already know you have asthma, you might not need any tests. Your doctor or nurse might be able to tell you have exercise-induced asthma based on your symptoms.
Or they might have you do a breathing test, such as:
● An "exercise challenge test" – This usually involves using a treadmill or exercise bike for several minutes, then doing a breathing test. This shows how your lungs are working.
● A test that involves breathing into a special medicine – You do a breathing test before and after inhaling a medicine. If you have asthma, the medicine will cause your airways to narrow.
Your doctor might also check for other problems that can cause similar symptoms. For example, people with vocal cord narrowing, lung disease, and some heart problems can have trouble breathing after exercising.
Should I avoid exercise?
No. Exercise is important for your health, even if you have asthma. But it might be better to avoid hard exercise on days when you are already having asthma symptoms.
How is exercise-induced asthma treated?
Treatment involves using a "quick-relief" medicine. This medicine opens the airway quickly. It comes in an inhaler, either a metered dose inhaler (figure 2) or dry powder inhaler (picture 1). Make sure you have your quick-relief inhaler with you anytime you plan to exercise.
The medicines to treat exercise-induced asthma are:
● Short-acting beta agonists ("SABAs") – These quickly relax the muscles in the airway. They are also called "short-acting bronchodilators." Examples include albuterol (sample brand names: ProAir HFA, ProAir RespiClick, Proventil HFA, Ventolin HFA) and levalbuterol (brand name: Xopenex HFA).
● Formoterol with an inhaled steroid – These quickly open the airway and also reduce inflammation in the airway. An example of this combination of medicines is budesonide with formoterol (brand names: Breyna, Symbicort.
Your doctor or nurse will tell you how and when to use the inhaler. For example, they might tell you to take 2 separate puffs to relieve symptoms. Take 1 puff with the first deep breath, and then 1 puff with the second deep breath. If you still have symptoms after 20 minutes, you can take 2 puffs again.
If you are having symptoms but don't have your inhaler, or if you still have trouble breathing after using it, call for an ambulance right away (in the US and Canada, call 9-1-1).
Some people feel shaky after taking a quick-relief inhaler. If this happens, talk to your doctor or nurse. They might switch you to a different medicine or lower your dose.
Can exercise-induced asthma be prevented?
Yes. First, it's important to take all of your asthma medicines exactly as instructed. Managing your asthma can lower your chances of having symptoms when you exercise.
You can also:
● Take medicine before exercising – This usually means using your quick-relief inhaler 5 to 20 minutes before exercising to help prevent symptoms. Most people use the same inhaler to treat and prevent exercise-induced asthma symptoms. But some people, such as children who are physically active many times a day, get another type of asthma medicine called a "leukotriene modifier." These come as pills and help reduce inflammation.
If you exercise most days of the week and need your quick-relief medicine each time, your doctor might suggest an asthma "controller" medicine, if you don't already take one. This helps prevent asthma symptoms from happening. You take it every day, even when you are not having symptoms. This way, you don't need the quick-relief medicine as often.
● Avoid exercising in certain conditions – Very cold, dry air can make symptoms worse. If you exercise outside on a very cold day, it might help to wear a loose scarf or mask over your nose and mouth. It can also help to avoid exercising in polluted air, or around pollen or mold if you are allergic.
● Warm up before you exercise – This might help prevent exercise-induced asthma.
Do not avoid exercise completely to prevent exercise-induced asthma. Exercise is important for staying healthy. Plus, regular exercise and better fitness can actually help reduce asthma symptoms. Your doctor or nurse can help you figure out what kind of exercise is best for you, and how to prevent and treat symptoms.
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Apr 27, 2026.
Topic 112887 Version 9.0
Release: 34.3.4 - C34.116
Images
figure 1: Asthma
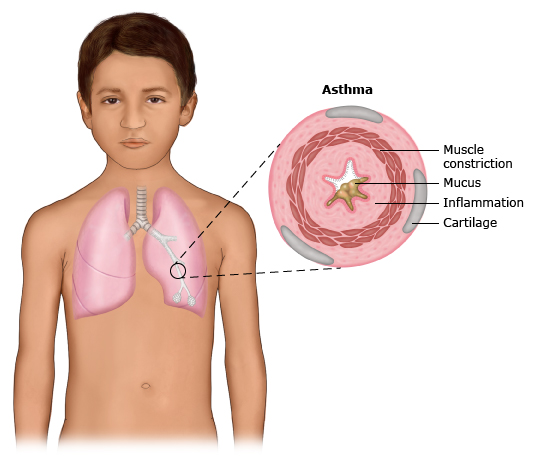
During an asthma attack or flare-up, the muscles around the airways tighten (constrict), and the lining of the airways gets inflamed. Then, mucus builds up. All of this makes it hard to breathe.
Graphic 65956 Version 11.0
figure 2: Adult using a metered dose inhaler
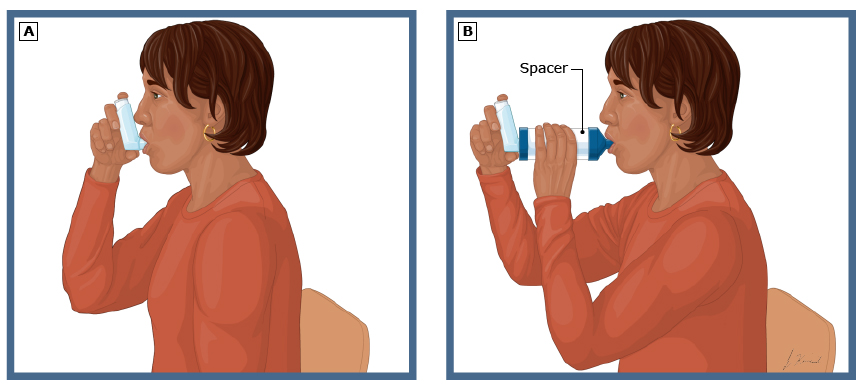
(A) Hold the MDI upright, with your thumb supporting the bottom of the inhaler.
(B) If you use a spacer, you might need to use your other hand to hold it. Different types of spacers are available.
Graphic 114257 Version 3.0
picture 1: Dry powder inhalers

These are examples of dry powder inhalers, or "DPIs." With this type of inhaler, the medicine is only pulled into a person's lungs when they take a deep, fast breath in from the inhaler. There are different styles of DPIs. Most are tube- or disk-shaped with a mouthpiece.
Reproduced from: How to use a dry powder inhaler fact sheet. National Heart, Lung, and Blood Institute 2021. https://www.nhlbi.nih.gov/resources/how-use-dry-powder-inhaler-fact-sheet (Accessed on January 10, 2024).
Graphic 143864 Version 1.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.