Health Library
Renovascular Hypertension Discharge Instructions
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
About this topic
One kind of high blood pressure is called renovascular hypertension. It happens when the blood vessels that supply the kidneys with blood become narrow, also known as renal artery stenosis. Different health problems can cause this. One of the main causes is when the blood vessels become blocked part of the way. The blockage may be caused by fatty deposits inside of the blood vessel.
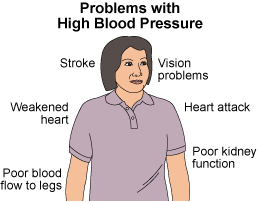
High blood pressure cannot be cured. You must control it with drugs and lifestyle changes. You may need a stent to open your renal artery to help the blood flow to your kidney. If you don’t control it, your high blood pressure can lead to heart attack, stroke, eye problems, and kidney problems.
Image(s)
What care is needed at home?
Ask your doctor what you need to do when you go home. Make sure you ask questions if you do not understand what the doctor says. This way you will know what you need to do.
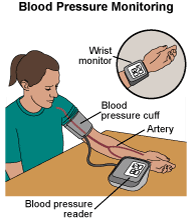
Learn how to check your blood pressure. Talk to your doctor about how often you should check it. Write down the numbers and let your doctor know what they are.
Ask your doctor or dietitian what changes you need to make to your diet. They may suggest that you:
Eat a healthy and balanced diet. Eat more fruits and vegetables.
Eat foods high in fiber and whole grains.
Eat foods low in fats and cholesterol
Eat foods low in salt and protein
Have drinks that are lower in caffeine
Check your weight more regularly
Stop smoking. Do not use illegal drugs.
Limit drinking beer, wine, and mixed drinks (alcohol).
Be active. Walk, garden, or do something active for 30 minutes or more on most days of the week.
Do not take any prescription or over the counter drugs without checking with your doctor first. They may raise your blood pressure.
What follow-up care is needed?
Your doctor may ask you to make visits to the office to check on your progress. Be sure to keep these visits.
What drugs may be needed?
The doctor may order drugs to:
Control blood pressure
Reduce cholesterol
Thin blood
Relax blood vessels
Reduce body fluids
Help with pain
Help with weight loss
Be sure to take all of your drugs as ordered. Do not skip doses or take double doses if you miss a dose.
Will physical activity be limited?
Ask your doctor about the right amount of activity for you.
What problems could happen?
Swollen area on the aorta. This is an aortic aneurysm.
Heart problems
Kidney problems
Stroke
Changes in eyesight
What can be done to prevent this health problem?
Keep a healthy weight and exercise regularly.
If you are overweight, try to lose weight by eating a better diet and exercising more often.
Control your blood sugar and cholesterol level.
Quit smoking, if you smoke.
Walk or do some form of physical activity on most days of the week.
When do I need to call the doctor?
Activate the emergency medical system right away if you have signs of a heart attack or stroke. Call 911 in the United States or Canada. The sooner treatment begins, the better your chances for recovery. Call for emergency help right away if you have:
Signs of heart attack:
Chest pain
Trouble breathing
Fast heartbeat
Feeling dizzy
Signs of stroke:
Sudden numbness or weakness of the face, arm, or leg, especially on one side of the body
Sudden confusion, trouble speaking or understanding
Sudden trouble seeing in one or both eyes
Sudden trouble walking, dizziness, loss of balance or coordination
Sudden severe headache with no known cause
Call your doctor if you have:
Blood pressure is 20 points higher than what you normally get on either the top or bottom number
Blood pressure that is higher than 220/120
Problems passing urine or blood in your urine
Swelling in your arms, hands, legs, or feet that is new or worse.
You are not feeling better in 2 to 3 days or you are feeling worse
Very bad headache
Severe pain in your upper back
Nausea or vomiting
Blood in your urine
Teach Back: Helping You Understand
The Teach Back Method helps you understand the information we are giving you. After you talk with the staff, tell them in your own words what you learned. This helps to make sure the staff has described each thing clearly. It also helps to explain things that may have been confusing. Before going home, make sure you can do these:
I can tell you about my condition.
I can tell you what my normal blood pressure should be.
I can tell you how I will check my blood pressure at home
I can tell you what I will do if I have signs of a heart attack or stroke.
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.