Health Library
Obstructive sleep apnea in adults
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
What is obstructive sleep apnea?
Obstructive sleep apnea, or "OSA," is a condition that makes you stop breathing for short periods while you sleep.
People with OSA do not know they stop breathing when they are asleep. But they do sometimes wake up startled or gasping for breath. They also often hear from loved ones that they snore.
With OSA, you stop breathing because your throat narrows or closes (figure 1). There is also another type of sleep apnea called "central" sleep apnea. In this type, you stop breathing because your brain does not send the right signals to your muscles to make you breathe. This is less common than OSA.
What are the symptoms of OSA?
The main symptoms are loud snoring, tiredness, and daytime sleepiness. Other symptoms can include:
● Restless sleep
● Waking up choking or gasping
● Morning headaches, dry mouth, or sore throat
● Waking up often to urinate
● Waking up feeling unrested or groggy
● Trouble thinking clearly or remembering things
Some people with OSA don't have symptoms, or don't realize they have them.
Should I see a doctor or nurse?
Yes. If you think you might have OSA, see your doctor.
Is there a test for OSA?
Yes. First, your doctor or nurse will ask about your symptoms. If you have a bed partner, they might also ask that person if you snore or gasp in your sleep. If the doctor or nurse suspects you have OSA, they might send you for a "sleep study."
Sleep studies can sometimes be done at home, but they are usually done in a sleep lab. For the study, you spend the night in the lab, and you are hooked up to different machines that monitor your heart rate, breathing, and other body functions. The study results tell your doctor or nurse if you have OSA.
How is OSA treated?
The most effective treatment is a device that keeps your airway open while you sleep. Treatment with this device is called "positive airway pressure," or "PAP." People getting PAP wear a face mask at night that keeps them breathing (figure 2). There are different types of PAP devices. The most common are "CPAP" and "APAP."
If your doctor or nurse recommends a PAP machine, be patient about using it. The mask might seem uncomfortable at first, and the machine might seem noisy, but using the machine can really help you. People with OSA who use a PAP machine feel more rested and generally feel better.
If PAP does not work, your doctor might suggest other treatment. Options might include:
● An oral device – This is a device you wear in your mouth. It is called an "oral appliance" or "mandibular advancement device." It helps keep your airway open while you sleep.
● Hypoglossal nerve stimulation – This involves a procedure to implant a small device into your chest. The device has a wire that connects to the nerve under your tongue. While you sleep, it sends an electrical signal that causes your tongue to push forward. This helps open up your airway.
● Surgery to widen your airway – This might involve removing your tonsils or other tissue in the throat that blocks the airway.
What else can I do on my own?
It might help to:
● Try to avoid sleeping on your back, if possible.
● Lose weight, if you have excess body weight – Your doctor can talk to you about how to do this in a healthy way. This might involve changing your diet or exercise habits and maybe weight loss medicines. Weight loss might help, but it does not cure OSA, and most people still need other treatment.
● Get regular physical activity – This might help you lose weight. But even if it doesn't, being active is good for your overall health.
● Avoid alcohol, especially in the evening – Alcohol can make OSA worse. Your doctor might also suggest avoiding certain "sedative" medicines that can make you sleepy.
Is OSA dangerous?
It can be. Risks include:
● Accidents – People with OSA do not get good-quality sleep, so they are often tired and not alert. This puts them at risk for car accidents and other types of accidents.
● Other health problems – Studies show people with OSA are more likely than others to have high blood pressure, heart attacks, and other serious heart problems. Some people also have mood changes or depression.
In people with severe OSA, getting treated (for example, with CPAP) can help lower these risks.
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Apr 18, 2026.
Topic 16178 Version 21.0
Release: 34.3.4 - C34.106
Images
figure 1: Airway in a person with sleep apnea
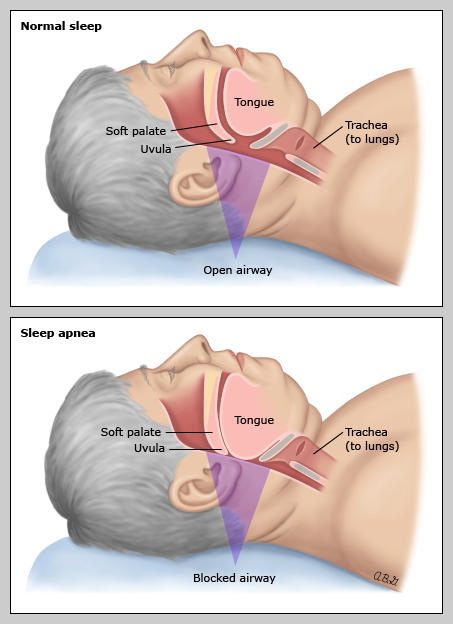
Normally, when a person sleeps, the airway remains open, and air can pass from the nose and mouth to the lungs. In a person with sleep apnea, parts of the throat and mouth drop into the airway and block off the flow of air. This can cause loud snoring and interrupt breathing for short periods.
Graphic 75747 Version 6.0
figure 2: Positive airway pressure ("PAP") for obstructive sleep apnea
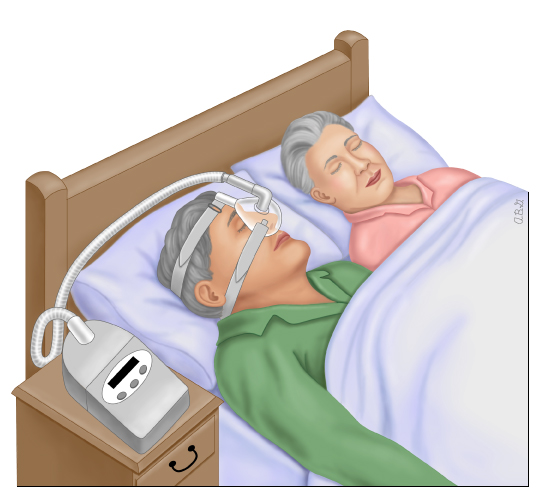
The PAP mask gently blows air into your nose while you sleep. It puts just enough pressure on your airway to keep it from closing. This mask fits over just the nose. Other PAP devices have masks that fit over the nose and mouth.
Graphic 65324 Version 6.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.