Health Library
Preeclampsia
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
What is preeclampsia?
This is a dangerous condition that can happen during pregnancy, usually in the second half (after 20 weeks). It can also happen during labor or soon after the baby is born.
People with preeclampsia have high blood pressure. They might also have too much protein in their urine, or problems with organs like the liver, kidneys, brain, eyes, or placenta. (The placenta is the organ that brings the baby nutrients and oxygen and carries away waste.) Also, the baby might not grow well and be smaller than normal.
What are the symptoms of preeclampsia?
Preeclampsia usually does not cause symptoms unless it is severe.
Signs and symptoms of severe preeclampsia include:
Bad headache
Changes in vision, like blurry vision, flashes of light, or spots
Belly pain, especially in the upper belly
If you have any of these symptoms, tell your doctor or nurse. These symptoms can happen in normal pregnancies and might not mean you have preeclampsia. But it's important your doctor knows about them.
How might preeclampsia affect my baby?
Preeclampsia can:
Slow the baby's growth
Decrease the amount of amniotic fluid around the baby (this is the liquid that surrounds and protects the baby in the uterus) (figure 1)
Is there a test for preeclampsia?
Yes. To test for preeclampsia, your doctor or nurse will:
Take your blood pressure
Check your urine for protein during pregnancy
Do blood tests to make sure your organs are working properly
When your doctor or nurse tells you your blood pressure, they say 2 numbers. For instance, they might say your blood pressure is "140 over 90." To be diagnosed with preeclampsia, your top number must be 140 or higher, or your bottom number must be 90 or higher. Also, you must have too much protein in your urine or certain problems with 1 or more of your organs.
It is possible to have high blood pressure (above 140/90) during pregnancy without having high protein in the urine or other problems. This is not preeclampsia. But your doctor will still watch you closely. You could develop preeclampsia or other problems related to high blood pressure.
How is preeclampsia during pregnancy treated?
For preeclampsia that develops during pregnancy, the only cure is to give birth. Your doctor or nurse will talk with you about whether it is better to have your baby right away, or to wait. The best decision depends on how severe your preeclampsia is and how many weeks pregnant you are. While giving birth to your baby will cure the preeclampsia, it's also important to give the baby as much time as possible to grow and develop.
If your preeclampsia is not severe:
If you are less than 34 weeks pregnant, your doctor will probably suggest waiting.
If you are between 34 and 37 weeks pregnant, your doctor will talk to you about your options and help you decide.
If you are more than 37 weeks pregnant, your doctor will probably suggest giving birth.
If you decide to wait, your doctor will check you and your baby often for any problems. You might need to stay in the hospital until it is time to give birth.
When it is time to give birth, you will probably get medicine to start contractions. This is called "inducing labor." Most people can have a vaginal birth. But in some cases, the doctor will need to do surgery to get the baby out of the uterus. This is called "cesarean birth."
If your preeclampsia is severe, you will probably need to give birth as soon as possible. You will also get medicine to lower your blood pressure, if it is very high. This helps keep you from having a stroke.
Rarely, people with preeclampsia have seizures. Your doctor or nurse might give you medicine during labor to prevent this.
How is preeclampsia after birth treated?
Preeclampsia can happen after giving birth, either again or for the first time. If had preeclampsia during pregnancy, or if you are at high risk, it's important to know the symptoms and when to call your doctor.
After birth, if you start having symptoms like a headache or blurry vision, or if your blood pressure gets very high, you will need treatment in the hospital. This might include:
Medicine given into a vein (by "IV") – This helps prevent seizures.
Medicine to lower blood pressure – This helps prevent a stroke.
You will need to stay in the hospital until your symptoms improve and your blood pressure returns to normal.
Can preeclampsia be prevented?
No. But it is very important you go to all the appointments you have with your doctor, nurse, or midwife. That way, they can find out as soon as possible if your blood pressure goes up, or if you have too much protein in your urine or any other problems.
If you are at high risk for preeclampsia, your doctor might have you take low-dose aspirin during your second and third trimesters of pregnancy (after 12 weeks). You are at high risk if you:
Had preeclampsia before, and your baby was born early
Are pregnant with twins
Have high blood pressure even when you are not pregnant
There are also other conditions that increase your risk. Your doctor can tell you if you are at high risk.
Do not take aspirin or other medicines, unless your doctor or nurse tells you it's safe.
Can preeclampsia cause other health problems?
If you had preeclampsia, you have a higher chance of getting high blood pressure and heart disease later in life. Tell your primary care doctor or nurse you had preeclampsia. They can talk to you about how you can lower your chance of getting these health problems in the future. This might include not smoking, eating healthy foods, keeping a healthy weight, and being active.
When should I call the doctor?
Call your doctor or nurse right away if you have any symptoms of severe preeclampsia, like:
Bad headache
Vision changes
Belly pain
New shortness of breath
You should also call if you are pregnant and:
Have any bleeding from your vagina
Notice your baby moving less than usual
Think you might be in labor
Images
figure 1: Pregnancy terms
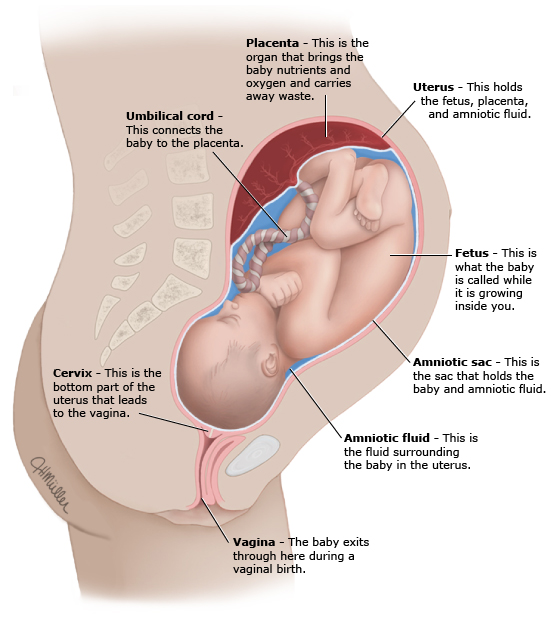
This drawing shows a baby inside the uterus late in pregnancy.
Graphic 82935 Version 8.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.