Health Library
Asthma in adults
You must carefully read the "Consumer Information Use and Disclaimer" below in order to understand and correctly use this information
The Basics
Written by the doctors and editors at UpToDate
What is asthma?
This is a condition that can make it hard to breathe. Asthma symptoms can be mild or severe. They can come and go. An asthma "attack" is when symptoms start suddenly. This happens when the airways in the lungs get more narrow and inflamed (figure 1).
Asthma can run in families.
What are the symptoms of asthma?
Symptoms can include:
● Wheezing or noisy breathing
● Coughing
● Tight feeling in the chest
● Shortness of breath
Symptoms can happen each day, each week, or less often. They can range from mild to severe. Although it is rare, an asthma attack can even lead to death.
Is there a test for asthma?
Yes. Your doctor will ask about your symptoms and have you do a breathing test to check how your lungs are working.
If your doctor thinks allergies might be making your asthma worse, they might suggest allergy testing. This can include skin tests or blood tests.
How is asthma treated?
Asthma is treated with different types of medicines that:
● Open the airway – This helps the muscles in the airway relax and lets air flow more easily.
● Reduce inflammation – This helps calm inflammation in the airway, which can help prevent asthma symptoms from happening.
The medicines can come as inhalers, liquids, pills, or shots. Your doctor might prescribe 1 or more depending on how often you have symptoms and how serious they are. They might change which medicine you take, and how much, over time.
There are 2 main types of asthma medicines:
● Quick-relief medicines – These open the airway quickly. They are used to treat asthma attacks. They can reduce symptoms in 5 to 15 minutes. Everyone with asthma should have a quick-relief inhaler to use during an asthma attack. Most people need them 1 or 2 times a week, or less often. But when asthma symptoms get worse, a person might need more doses.
● Long-term controller medicines – These help reduce inflammation in the long term. This can help prevent asthma symptoms from happening. Not everyone with asthma needs these. But those who need controller medicines take them 1 or 2 times a day every day, even if they have no symptoms. You might need a controller medicine if, for example, you have asthma symptoms more than 2 times a week. When these medicines are working well, your asthma symptoms are managed, and you should not need quick-relief medicines very often.
When these medicines are put into inhalers, many people have 1 inhaler for quick relief and 1 for long-term control. A person might use 1 inhaler for both.
It is very important to take all the medicines exactly as your doctor prescribes. You might take medicines a few times a day. Your doctor, nurse, or pharmacist will show you how to use your inhaler(s).
If your symptoms get much worse all of a sudden, use your quick-relief medicine and contact your doctor or nurse. You might need treatment in the hospital.
What is an asthma action plan?
This is a list of instructions that tell you (form 1):
● Which medicines to use each day at home
● Which medicines to take if your symptoms get worse
● When to get help or call for an ambulance
If you have frequent or severe asthma symptoms, your doctor might suggest you have an asthma action plan. If so, you and your doctor will work together to make one. As part of your action plan, you might need to use a "peak flow meter." Breathing into this device shows how your lungs are working. Your doctor will show you how to use it.
How can I prevent asthma symptoms?
There are things you can do to help prevent asthma attacks. Your doctor or nurse can talk to you about what is most important for you.
In general, you should:
● Avoid "triggers" – These are things that make your symptoms worse. Common triggers include smoke, air pollution, dust, mold, pollen, strong chemicals or smells, and very cold or dry air. Being around certain animals might trigger symptoms. Exercise and stress can also be triggers. But you should not avoid exercise to avoid triggering your asthma. This is because exercise is important for staying healthy. Plus, regular exercise and better fitness can actually help reduce asthma symptoms.
Some adults with asthma have worse symptoms if they take aspirin or "NSAID" medicines. NSAIDs include ibuprofen (sample brand names: Advil, Motrin) and naproxen (sample brand name: Aleve). Ask your doctor if you need to avoid these.
If you can't avoid certain triggers, talk with your doctor about what you can do. For example, you might need to take an extra dose of your quick-relief inhaler medicine before exercising or being around things you are allergic to.
● Lower your risk of getting sick – Some infections can make asthma symptoms worse. These include colds, the flu, and COVID-19.
It's important to get the COVID-19 vaccine. This lowers the risk of severe illness if you do get COVID-19. You should also get a flu shot every year. Plus, some people need to get a vaccine to help prevent pneumonia.
If you think you might have an infection, tell your doctor or nurse. They can help you decide if you need treatment.
● Make sure you know how and when to take your medicines – If you take controller medicines, follow all instructions to help prevent symptoms. You should also make sure you know how and when to use your quick-relief medicine.
● See your doctor or nurse regularly – If you need asthma medicine every day, see your doctor or nurse at least every 6 months. At these visits, they will ask about your symptoms, check how your lungs are working, and discuss your treatment plan. People with severe asthma and frequent asthma attacks should see a doctor who specializes in asthma.
What if I want to get pregnant?
Talk to your doctor about how to manage your asthma. Keeping your asthma well managed is important for the health of your baby. Most asthma medicines are safe during pregnancy.
When should I call the doctor?
Call for an ambulance right away (in the US and Canada, call 9-1-1) if you have severe symptoms like:
● You have so much trouble breathing you cannot talk.
● Your lips or fingernails turn gray or blue.
Call your doctor or nurse if you:
● Have an asthma attack and the symptoms do not improve, or get worse, after using a quick-relief medicine
● Need to use your quick-relief medicine more than a few times a week
● Cannot do your normal activities because of your asthma symptoms
● Have any questions about your medicines
All topics are updated as new evidence becomes available and our peer review process is complete.
This topic retrieved from UpToDate on: Apr 04, 2026.
Topic 15343 Version 32.0
Release: 34.3.4 - C34.92
Images
figure 1: Asthma
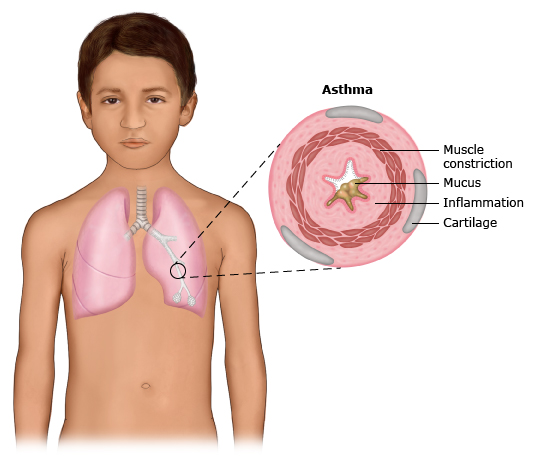
During an asthma attack or flare-up, the muscles around the airways tighten (constrict), and the lining of the airways gets inflamed. Then, mucus builds up. All of this makes it hard to breathe.
Graphic 65956 Version 11.0
form 1: Asthma action plan (adult)
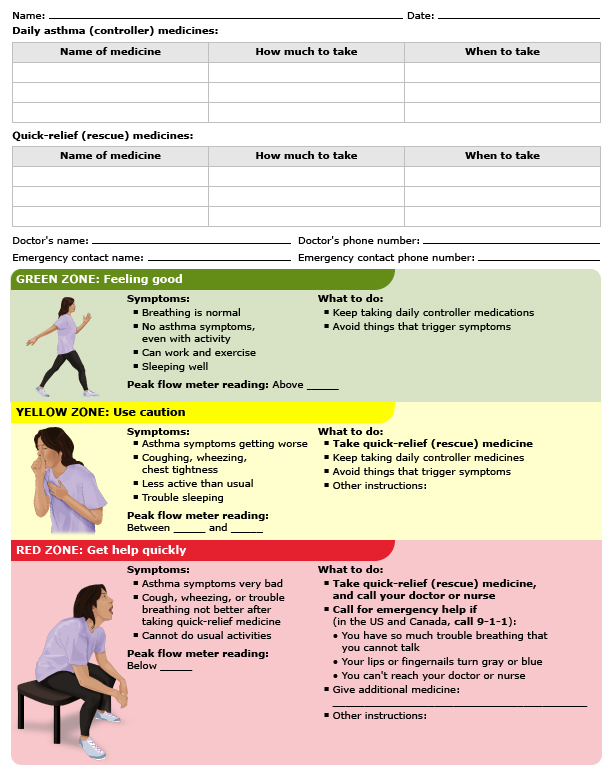
An asthma action plan is a list of instructions that tell you:
What medicines to take at home each day, if any
What symptoms to watch for
What other medicines to take if your symptoms get worse
When to call the doctor or get emergency help
Graphic 140838 Version 2.0
Give to a Healthier Future
Help us elevate and expand our care, make breakthroughs in biomedical science and improve community health and wellness.
Healthier communities. Healthiest lives. Together.