Program Overview
The Neonatal-Perinatal Medicine Fellowship at the University of Vermont Medical Center is a close-knit, academically rigorous program which aims to foster the development of excellent academic neonatologists through an emphasis on clinical care of critically-ill newborns, research, and teaching.
To meet this aim, we provide a comprehensive three-year curriculum comprised of didactic and experiential learning. Fellows are expected to think critically and gain expertise in scholarly activity during throughout their training. Neonatal-Perinatal Medicine and Larner College of Medicine faculty work with fellows to establish a Scholarship Oversight Committee and delineate a research plan during the first year of training. Additional faculty from Vermont Oxford Network (VON) and the Cochrane Collaboration provide direct mentoring and teaching. Our fellows participate in and lead quality improvement projects and author Cochrane Neonatal Reviews as a core part of their training. As a small fellowship training program, scholarly activity is individualized to meet each fellow's career and research goals. Fellows in our program are actively engaged in clinical, translational, and global health research in Vermont and throughout the world. Along with the American Board of Pediatrics we support fellow involvement in global health research, and we work in close collaboration with VON and other non-profit organizations directed at improving health for neonates around the world.
Our rural setting and network-based hospital system allows for unique experiences with neonatal developmental and medical follow-up as well as transport medicine. Our program combines the strength of bigger academic centers with the flexibility to work closely with attendings who are nationally and internationally known. Upon completion of the program, fellows are-prepared for both academic and non-academic careers in Neonatal-Perinatal Medicine.
A Brief History of Our Program
The NICU at the University of Vermont was established in the early 1960's by Dr. Jerold F. Lucey, one of the fathers of modern Neonatal-Perinatal Medicine. The importance of regionalization, particularly in a rural state like Vermont, proved life-saving and visionary. Although a small program, the University Of Vermont Division Of Neonatal-Perinatal Medicine has made a large contribution to the field.
As a pioneer in neonatal care, Professor Lucey was known for the seminal work regarding the use of phototherapy to prevent kernicterus in infants with jaundice and was responsible for the introduction of transcutaneous oxygen monitoring. He also helped organize many of the first clinical trials of surfactant in the prevention and treatment of respiratory distress syndrome. After the early surfactant trials, the University of Vermont was an original member of the NICHD Neonatal Network and the founding member of the Vermont Oxford Network, a voluntary collaboration of neonatal intensive care units formed to improve the care of newborns worldwide. Under the leadership of faculty member Jeffrey Horbar, VON has become the premier worldwide network in quality for newborn care.
The UVM Medical Center NPM Fellowship Today
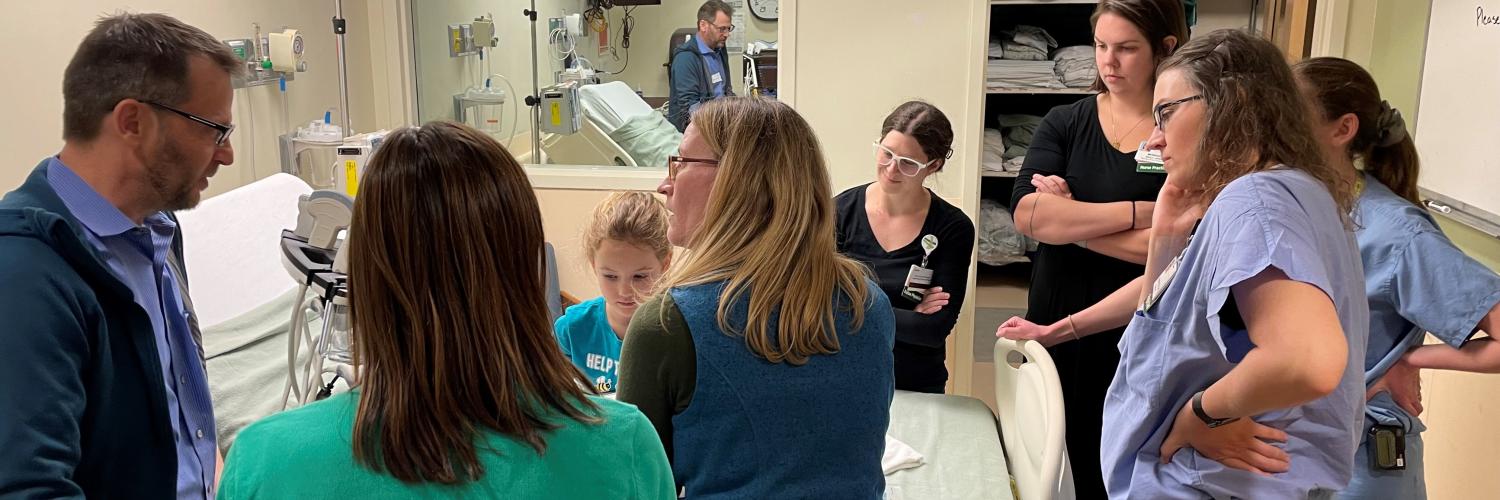
Our 29-bed NICU is the only level III unit in Vermont, with a new single room-based unit currently in the planning stage. Our division includes nine board-certified neonatologists, three NPM fellows, and 13 advanced practice providers. Our neonatal-perinatal subspecialty fellowship training program is directed by Aaron Wallman-Stokes, MD, with Dr. Deirdre O'Reilly serving as the Associate Program Director as well as the Chief of the Division of Neonatal-Perinatal Medicine. Whittney Barkhuff, MD, PhD is the unit’s Medical Director. Our faculty prides itself on fostering a learning environment where critical thinking, open and respectful discussion and the practice of evidence-based medicine are prioritized. We are a tight-knit group with diverse backgrounds and interests but a shared goal: mentoring future neonatologists capable of providing excellent clinical care, producing impactful scholarly work and carrying forward a passion for teaching and lifelong learning.
Thank you for your interest in our program. Please contact us with any further questions or submit an application through ERAS.