Cataract Surgery
Surgery Overview
Cataract surgery helps you see better. It replaces your natural lens, which has become cloudy, with a clear artificial one.
Types of cataract surgery include:
- Phacoemulsification. This is the most common type of surgery. The doctor makes a small cut in your eye and uses an ultrasound tool to break your cloudy lens apart. The small pieces of the lens are removed and replaced with an artificial lens.
- Extracapsular extraction. This uses a larger cut to remove the lens in one piece. It is replaced with an artificial lens.
- Femtosecond laser-assisted cataract surgery (FLACS). This uses laser technology and replaces the natural lens with an artificial lens.
Before surgery, you may be given medicine to help you relax. Medicine will be used to numb your eye. After surgery, you may have a bandage or shield on your eye.
Most people will see better in 1 to 3 days.
How It Is Done
How a cataract looks
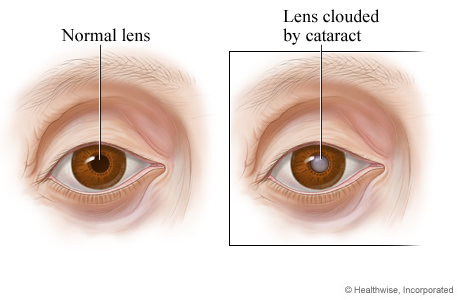
In a normal eye, the lens—which lies behind the pupil—is clear (transparent), so the pupil appears black. In an eye with a cataract, the pupil may look gray. This is because the natural lens has become cloudy, which may affect vision.
Close-up of a cataract
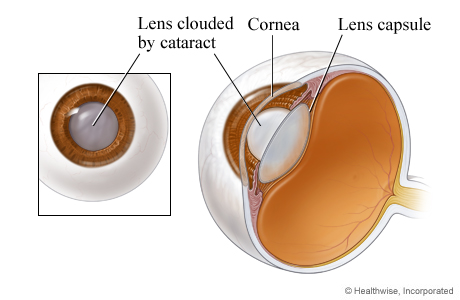
The cornea is the clear layer that covers the front of the eye. The lens is contained inside the eye's lens capsule. A cataract is a partial or complete cloudiness in the lens.
Incision for surgical instrument is made
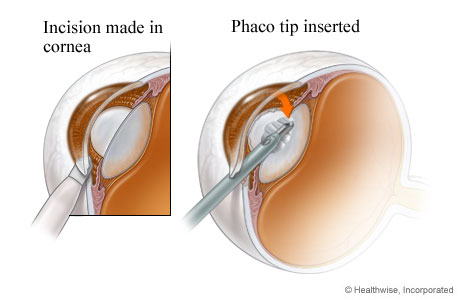
A small cut (incision) is made in the eye so a small instrument (phaco probe) can reach the cataract.
Lens is broken up and removed
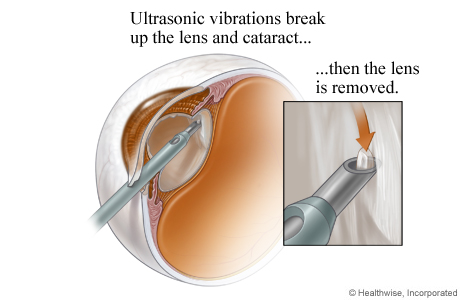
The probe uses sound waves (ultrasound) to break the cataract into small pieces. Then the surgeon uses suction to remove the cataract from the eye.
Intraocular lens (IOL)
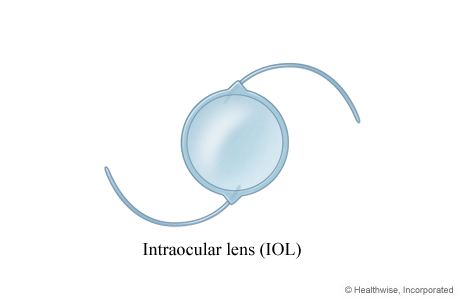
A variety of artificial lenses (intraocular lenses or IOLs) are available to replace your natural lens. Your doctor can help you choose the type that may work best for you.
A lens replacement (IOL) is inserted
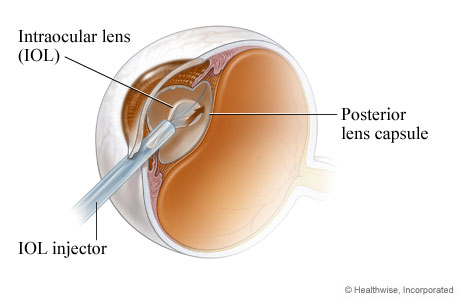
After the cataract is removed, an intraocular lens (IOL) may be placed inside the lens capsule. The back of the lens capsule (posterior capsule) keeps the IOL in place.
Intraocular lens in place
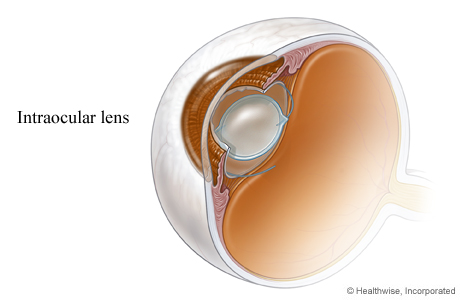
The intraocular lens (IOL) takes the place of the eye's natural lens. The incision does not usually require stitches.
Before and after cataract surgery
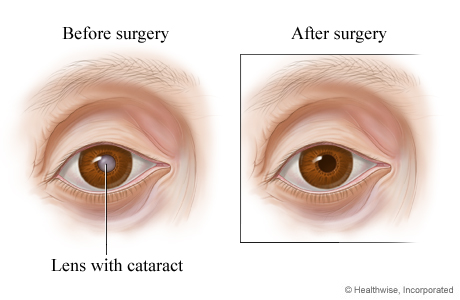
Before cataract surgery, the cloudy lens can be seen through the pupil. After cataract surgery, the pupil appears black because the intraocular lens is clear.
Learn more
What To Expect
Before you leave the outpatient center, you will get the immediate eye care that you need after surgery. The surgeon will review the symptoms of possible complications, eye protection, activities, medicines, and required visits. They will also tell you what to do for emergency care if you need it.
The eye that was operated on may be bandaged for 1 night after surgery. You may wear a protective shield over the eye at night for about a week. There is normally no significant pain after surgery.
You most likely will need to see the doctor for checkups 1 or 2 days after surgery, and again within a few weeks after surgery. If you have any complications, you should visit sooner and more often.
Most people get a new eyeglass prescription about 6 weeks after surgery.
Why It Is Done
The decision to have this surgery is based on whether:
- Your work or lifestyle is affected by vision problems caused by the cataract. For example, you may want surgery if you need to drive, especially at night.
- Glare caused by bright lights is a problem.
- You have another vision-threatening eye disease, such as diabetic retinopathy or macular degeneration.
How Well It Works
Cataract surgery is successful for most adults. Surgery may also improve vision in infants who have cataracts.
Both phacoemulsification cataract surgery and femtosecond laser-assisted cataract surgery (FLACS) work about equally well for treating cataracts in adults. FLACS is more expensive, but it may be a better option in some cases. For example, people who are going to have multifocal lenses placed may choose FLACS.
People who have surgery for cataracts usually have:
- Improved vision.
- Increased mobility and independence.
- Relief from the fear of going blind.
Risks
Although the risk is low, surgery for cataracts does involve the risk of partial to total vision loss if the surgery is not successful or if there are complications. Some complications can be treated and vision loss reversed, but others cannot. Complications that may occur with cataract surgery include:
- A torn lens covering (posterior capsule rupture).
- Infection in the eye (endophthalmitis).
- Swelling and fluid in the center of the nerve layer (cystoid macular edema).
- Swelling of the clear covering of the eye (corneal edema).
- Bleeding in the front of the eye (hyphema).
- Detachment of the nerve layer at the back of the eye (retinal detachment).
Complications that may occur some time after surgery include:
- Problems with glare.
- Clouding of the back portion of the lens covering (capsule) that remains after surgery. (Your doctor can easily treat this using a laser.)
- Retinal detachment.
- Glaucoma.
- Astigmatism or strabismus.
- Sagging of the upper eyelid (ptosis).
Credits
Current as of: June 5, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: June 5, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.
To learn more about Healthwise, visit Healthwise.org.
© 1995-2024 Healthwise, Incorporated. Healthwise, Healthwise for every health decision, and the Healthwise logo are trademarks of Healthwise, Incorporated.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.














